Scientists have discovered a new factor in the effective delivery of drugs in the tumor

Scientists conducted an intravital (on living tissue) study of the mechanism of targeted drug delivery to malignant tumors using liposomes. It turned out that the immune cells of the body neutrophils 30% increase the efficiency of drug delivery to the tumor.
Liposomes – artificially created fat vesicles – penetrate the tumor due to the so-called enhanced permeability and retention (EPR) effect. Inside the liposomes, the medicine is “sutured”, and when it enters the malignant tissue, it is released.
The EPR effect occurs due to the excessive growth of blood vessels caused by the abnormal need of the tumor for oxygen and nutrition. With pathological growth, huge pores up to 200 nm in diameter appear in the walls of the vessels. Also, the growth of the tumor causes compression of the lymphatic vessels and prevents the normal outflow of intercellular fluid. Thus, liposomes penetrate the tumor and cannot exit due to impaired lymphatic drainage.
It is believed that due to the EPR effect, liposomes can penetrate only into the tumor, but not into healthy tissues. But is this really so? And what happens in the vessel?
In the course of the study, scientists observed the delivery of the drug to the tissues of healthy mice and to various types of malignant tumors: breast cancer, prostate cancer, and melanoma. The observations were carried out using an intravital microscope, which allows you to study processes directly in a living organism.
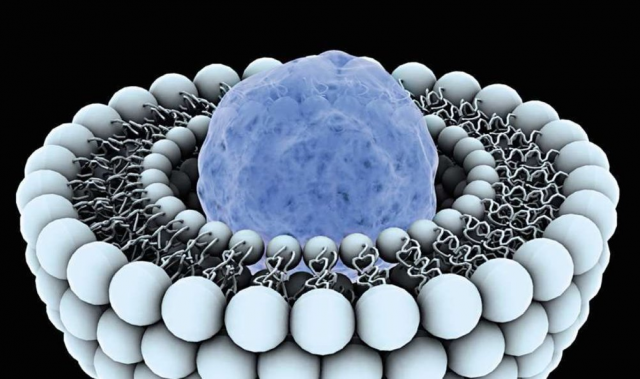
Liposomes "clinging" to a cancer cell
“The first conclusion we received as a result of the study is that two types of penetration of liposomes from blood vessels into tissues occur in living tissues. A microleak is a small isolated accumulation of liposomes around a vessel. Such a process is useless for the treatment of tumors, as it does not allow the drug to reach the tumor cells. Moreover, micro-leaks were found in healthy tissues, which explains the toxicity of liposome-based drugs used in a modern clinic, ” tells the author of the work, a researcher at the laboratory "Biomedical nanomaterials" NUST "MISiS" Victor Naumenko.
The second, most interesting observation result is neutrophil, a type of white blood cell, and the body’s immune cell that leaks into the tumor tissue. When the neutrophil leaves the vessel, along with it, through the “ajar door” in the vascular wall, liposomes manage to penetrate into the tumor. According to the results obtained by the scientific team, neutrophils increase the efficiency of penetration of liposomes into the tumor by a third.
This discovery gives a clear pattern: neutrophils increase the vascular permeability of the tumor for targeted delivery of liposomal drugs, and therefore increase the chance of cure. Moreover, this happens only in the case of a macro leak, which is a large diffuse “cloud” of liposomes that penetrates deep into the tumor, thereby ensuring targeted drug delivery.
“Distinguishing between two types of leaks is important in understanding the mechanism of how liposome-based drugs work. Our results indicate that micro-leaks not only do not contribute to the delivery of drugs to tumor cells, but are also responsible for its unwanted accumulation in healthy tissues. The therapeutic effect is achieved due to macroleakings, and neutrophils can help strengthen it, ”- stressed Victor Naumenko.
The team is currently continuing laboratory studies to reduce the unwanted side effects of liposome therapy. The development of artificial stimulation mechanisms for the production of neutrophils in the patient’s body to enhance oncotherapy is one of the promising areas of application of the obtained data.